When President Trump advocated reopening the economy, he warned that the lockdowns might have more of an adverse impact than COVID-19. Some assumed he was only talking about the economic implications but he also noted the risk of drug overdoses and suicides. We have seen increases in both of those types of deaths, along with significant mental health impacts.
However, the tragedy of extended lockdowns is compounded by people not seeking medical care.
The United Kingdom is noting this trend in raw numbers. From The Telegraph:
Unexplained deaths in private homes are nearly nine times higher than those from Covid-19 amid fears that many people are still not accessing life-saving medical treatment.
The latest figures from the Office for National Statistics (ONS) show that there were 830 excess deaths at home in the week ending September 4 compared to the five-year average. In contrast, just 99 people died with coronavirus mentioned on the death certificate in the same period. Only seven of those died at home.
The figures also show that there were 371 fewer deaths in hospitals, suggesting hundreds of people who would normally have been taken in for treatment had died at home instead.
Even accounting for that number, it still means there are around 450 excess deaths a week at home, from unknown causes, of people who may not ordinarily have died.
Recent studies have shown that many people did not seek help for serious conditions, such as heart attacks, in recent months.
Trump Was Right: The COVID-19 Lockdowns Are Driving Young People to Suicidal Thoughts
The article warns of the risks associated with the first lockdown, now that Europe may be experiencing a resurgence of cases. In the last eight weeks, 1,117 death registrations listed COVID-19 as a cause. Excess deaths at home were 5,556, leading some medical experts to warn the COVID-19 response is now more deadly than the virus.
As of April, 87% of cancer surgeons in the U.K. had stopped or reduced the number of procedures they were doing. Experts have estimated this could lead to an increase of 20% in cancer deaths. Because of the socialized system, the backlog is immense, and the results may get worse. The article notes that surgeons would have to work at 160% of their capacity to clear the backlog.
While no one has compared excess deaths at home in the United States recently, we know that emergency room visits for acute issues such as strokes and heart attacks were down 42% from March 31 through April 27. In the full ten weeks following the declaration of the COVID-19 national emergency, visits were still down for life-threatening conditions:
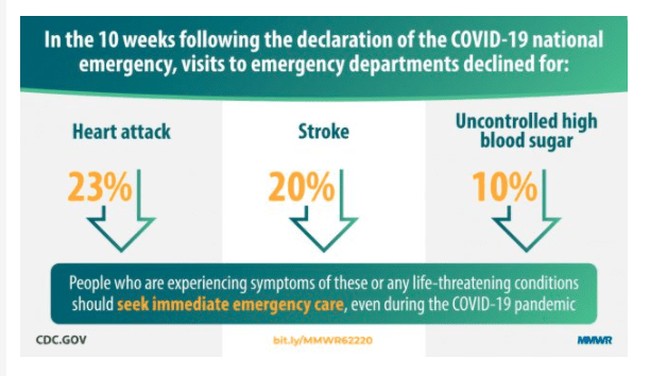
Someone in the United States has a heart attack every 40 seconds, or nearly 790,000 per year. Likewise, strokes affect approximately 795,000 people, and there are 34 million Americans with diabetes. Yet as of September 11, we know four in ten adults, often those with preexisting conditions, avoided medical care:

Studies have also shown cancer screenings are down, which may lead to an increase in deaths where timely screening would have saved a life:
According to the Prevent Cancer Foundation, 35 percent of Americans had a cancer screening scheduled during the pandemic and missed it. Similarly, a survey this summer by the medical technology company Hologic found more than a quarter of women plan to either skip or delay their annual screenings this year. That includes mammograms, which can help catch breast cancer early when it’s easier to treat.
As a result, the National Cancer Institute estimates that there could be 10,000 additional breast and colorectal deaths over the next decade as a result of missed screenings and delayed diagnoses, and health experts are raising concerns.
Did a Math Error Lead to the Never-Ending COVID-19 Lockdowns?
Now we have some insight into the death rates by age throughout the pandemic from the CDC. Phil Kerpen from American Commitment was kind enough to calculate them by age. He also noted that these calculations are based on early experience in Europe, and survival rates have been improving:
CDC estimated survival rates by age:
0 to 19: 99.997%
20 to 49: 99.98%
50 to 69: 99.5%
70+: 94.6% https://t.co/9UrhHFqVhM— Phil Kerpen (@kerpen) September 22, 2020
As a reminder, the infection fatality rate (IFR) for the seasonal flu, according to the World Health Organization, is 0.1%. For ages birth to 49, the COVID-19 IFR is lower than for the seasonal flu. This fact needs to start guiding public policy nationwide immediately, especially regarding school openings, where the average age of teachers is 41.
Clearly, those most at risk are over 70, and we know that these deaths generally include those with preexisting conditions. As of June, almost half of all deaths from COVID-19 had occurred in nursing homes. A study published in 2010 showed that the median length of stay in a nursing home before death was five months. Sixty-five percent passed away within one year. As has been noted previously, it is very likely that those who died in nursing homes would have died in the near term. This factor is why the excess deaths for the year matter.
Yet, much younger, healthier people are at risk due to lower levels of preventative care, screenings, and even delays in treating chronic conditions and diagnosed cancers. One CDC analysis showed shocking decreases in the number of heart catheterizations done during the pandemic, meaning there are significantly more people with severe artery blockages walking around.
Lies, Damn Lies, and COVID-19 Statistics
An interactive graph from the Heritage Foundation also shows 1.6% of counties in the United States have experienced nearly 50% of the deaths. Yet in vast swaths of the country, draconian measures remain. Children are still home, and college students are subjected to meaningless testing.
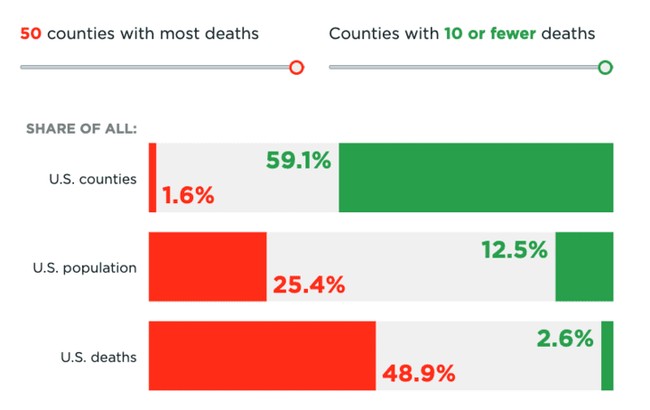
Yelp says 60% of closures on their platform are permanent, yet Democrats in Congress refuse to vote on a narrow relief bill.
If the goal is to save “just one life” as Governor Andrew Cuomo famously said, public policy needs to be reevaluated now. Because it is becoming clear that the years of life lost to the lockdown will far exceed the years of life lost to COVID-19. And this is the measure all public policy should be based on.










Join the conversation as a VIP Member