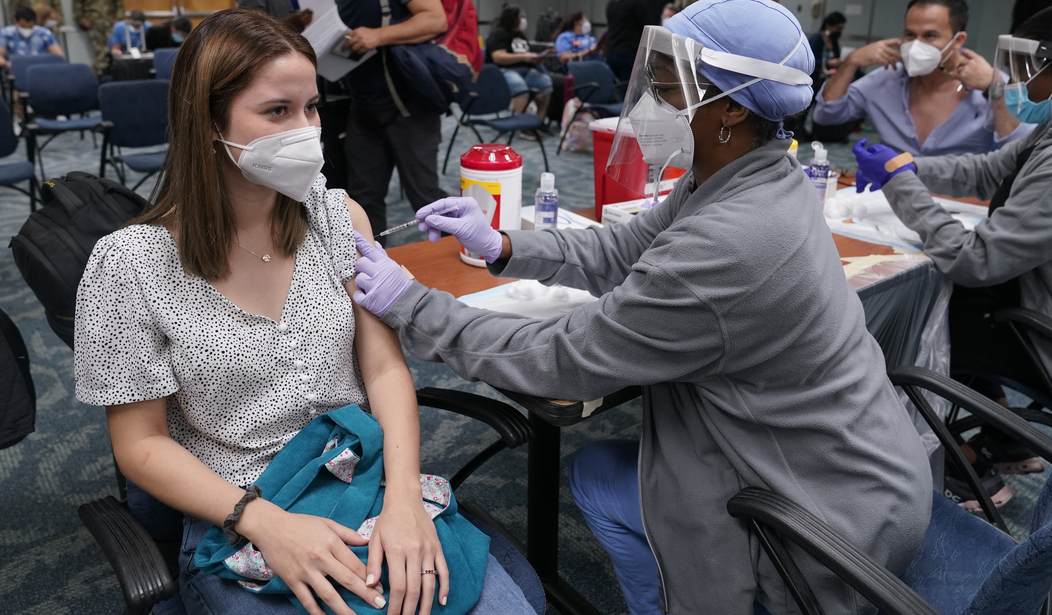
Initial data on breakthrough infections for the COVID-19 vaccines were highly encouraging. According to the CDC, through April 15, 2021, a vanishingly small number of fully vaccinated individuals later tested positive for COVID-19. Roughly one in a million died. Upon full investigation, some of these numbers improved because of patients who tested positive for COVID-19 due to hospital admission for another health problem but never suffered from symptoms of the virus.
The CDC has stopped collecting data on breakthrough infections unless the person is hospitalized or dies beginning May 1. According to initial data from April, this means they would have detected 6.8% of breakthrough cases. Globally, confirmed reinfections remain very low for patients who have recovered from COVID-19. Data for the U.S. is hard to come by because our health bureaucracy doesn’t like to admit the recovered have any immunity. That is news that decreases the likelihood you will get jabbed.
So, it will be impossible to tell if the data in the U.S. mirrors the data coming out of Israel regarding the Delta variant. According to the latest data from the Israel Ministry of Health:
According to updated data from the Ministry of Health, the effectiveness of the vaccine against infection has dropped to 64% in the last month, against the background of the spread of the Delta strain and the abolition of restrictions. However, the protection against serious illness and hospitalization is still very high. Senior epidemic treatment team member: “Disturbing data”. In the staff discussion tonight, no decision was made regarding a third vaccine.
It is important to note that Israel has a nationalized health service with centralized data collection, making its outcome data far more reliable than the CDC’s. The country also uses the Pfizer vaccine exclusively. While both the Pfizer and Moderna vaccines use mRNA technology, that does not mean every outcome will be the same. There will not be any way to assess a similar trend for the Johnson and Johnson vaccine. It uses a different delivery technology, and it is not in use in Israel.
Three days ago, 61% of Israelis had received at least one injection, and the country is working to vaccinate those over the age of 12. Limitations on vaccinating younger Israelis affect the percentage because the country has one of the youngest populations globally. Before June, Israel was reporting vaccine effectiveness of nearly 95%.
The Pfizer vaccine is still 93% effective in preventing severe illness. Because deaths lag, any assessment on mortality would be premature. It took two months from first detecting the variant in mid-April to the first outbreak in mid-June. Now 90% of cases are caused by the Delta variant.
Israel’s Ministry of Health is considering a third vaccination recommendation. It is not clear what they believe this could provide. Researchers developed the mRNA vaccines based on the mapping of the Wuhan version of COVID-19, which was gone in its original form by the time vaccines were in the trial phase. The spike used in the mRNA technology will not encourage different immune responses than it already has. If the Delta variant has learned to evade that immunity to cause primarily mild disease, the benefit seems dubious.
Missing from the current write-ups of the preliminary report is any data on recovered patients. In the initial rollout, Israel treated recovered patients as vaccinated to issue passports. It appears the current information only takes the vaccinated population into account. It would be interesting to know if there is any difference between rates of illness prevention in that population.
However, the new data leads to a critical question: Are the COVID-19 vaccines a true immunologic? Examples of these would be the vaccine you receive as a youngster that provides sterilizing immunity after multiple doses and usually a booster in your teens. Or are they therapeutics like the annual flu shot? The protection against influenza is nowhere near 100% because development is a predictive model based on surveillance for different strains. However, this makes a course on influenza less severe for many who take it.
That calculus matters, given the risks of the current vaccines, especially for young people. Reviewing CDC data after reports about heart-related side effects in young men, Alex Berenson found some interesting numbers:
Also keep in mind that heart inflammation is only ONE potential problem the vaccines may cause. The CDC and journalists generally like to compare each individual vaccine side effect to ALL the risks of Covid, a slight-of-hand [sic] that has the effect of making the vaccines seem safer.
In fact, the CDC’s own data shows that for every 100,000 vaccines given to young people, more than 25,000 will have temporary side effects that prevent them from “normal activities,” 700 will require medical care and 200 will be hospitalized.
The hospitalization rate post-vaccine that Berenson found is far higher than what the CDC reported with COVID-19 for those 12-17:
COVID-19 adolescent hospitalization rates from COVID-NET peaked at 2.1 per 100,000 in early January 2021, declined to 0.6 in mid-March, and rose to 1.3 in April. Among hospitalized adolescents, nearly one third required intensive care unit admission, and 5% required invasive mechanical ventilation; no associated deaths occurred.
What exactly is the risk-reward calculation that makes a case for vaccinating those under 18? Under 18 is a population that rarely becomes severely ill from COVID-19 and has near-zero mortality rates. Why would our public health experts encourage what may become a therapeutic with such a high rate of severe side effects in that population? It is certainly something to consider before vaccinating any child under 18.